Table of Contents
▼What Is the Medical Billing Process?
The medical billing process is a crucial system to convert healthcare services into a practice’s cash flow. In this blog, you will gain a clear understanding of how the medical billing process works from start to finish. We will walk you through the essential stages, along with the patient registration’s role in affecting the billing cycle.
This blog will provide a clear demonstration of how claims reach payers. You will learn how the providers manage denials and resolve outstanding balances for timely payments. By the end of this article, you will gain insight into a successful billing process with the help of key performance metrics.
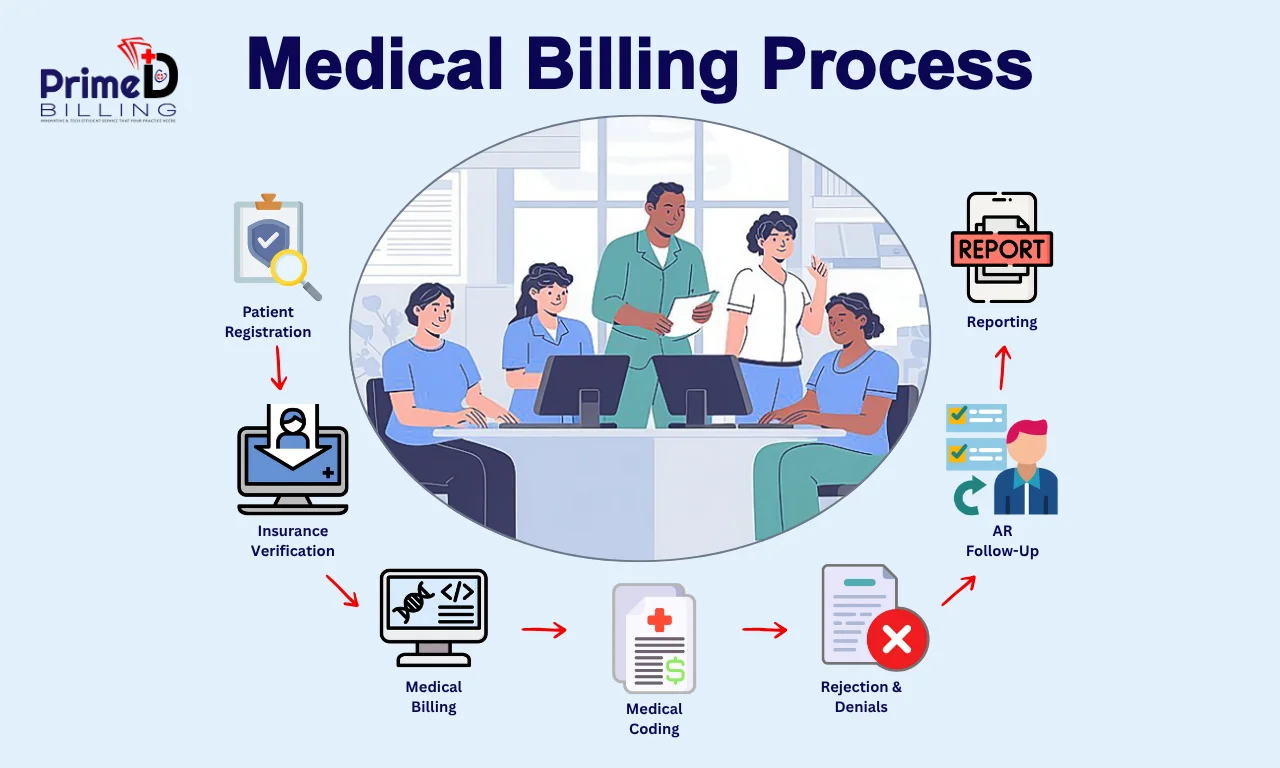
What Are the Main Steps of the Medical Billing Process?
The medical billing cycle starts from when a patient books their appointment. It continues until the payment of the accurate outstanding balance. Here’s a step-by-step guide on how the medical billing cycle works:
Patient Registration
The first step involves collecting patient insurance information along with the demographics. Accurate intake registration reduces the chances of claim errors or denials. Incorrect or missing information may affect the entire billing cycle process.
Insurance Verification
Medical billers perform insurance verification before the start of patient treatment. It is essential to identify:
- Coverage limitations
- Co-payments
- Deductibles
- Coinsurance
- Pre-authorization
- Insurance policy status
- Services covered
Medical Coding
Medical coders translate the patient’s diagnosis and treatment plan into standardized code. They can do it during the patient’s visit or after they have left. Incorrect or mismatched coding can lead to denials, audits or compliance issues. There are three main types of codes:
- CPT (Current Procedural Terminology)
- ICD-10 (International Classification of Diseases)
- HCPCS (Healthcare Common Procedure Coding System)
Charge Entry
It refers to assigning the codes to appropriate charges. These charges depend on the providers’ fee schedule. Charge entries determine the financial value of a patient and provider encounter. The biller must match them with the correct codes to ensure proper reimbursement.
Claim Submission
Medical billers initially compile the claim after the charge entry process. After that, they submit it either directly to insurance companies or through clearinghouses. The clearinghouses check for errors and correct them before submitting.
The insurers process cleaner claim submissions more quickly. Whereas, missing or inaccurate data can lead to rejection or denials.
Payment Posting
After the insurance companies review claims, they send payment postings to providers via ERA. This explains the paid, adjusted or denied amount to the providers. The insurers post these payment details into the providers’ billing system for an accurate record.
Denial Management
If a claim is denied, the medical biller must review and correct it. They may also file for an appeal if necessary. There are several reasons for claim denials, a few of them are:
- Missing documentation
- Eligibility issues
- Incorrect coding
- Lack of authorization
The medical billers consistently follow up on the claims to recover the practice’s revenue.
AR Follow-Up
Some claims get lost in the process and remain unpaid. AR Follow-up ensures that no claim is left behind to improve the cash flow of a healthcare practice. The AR Follow-up process involves:
- Contacting payers for delayed responses
- Following up with patients for outstanding balances
- Tracking unresolved claims
- Resolving error issues
-
How Does Patient Registration Affect the Billing Cycle?
Patient registration is the foundation of the entire medical billing cycle. Medical billers treat this step as a mission-critical input. They ensure quality checks and seamlessly integrate with front office workflows for a smooth process.
-
Accurate Patient Demographics
-
Effect on Claims
Incorrect or incomplete patient demographics can lead to claim denials. Even a minute error creates mismatches in the payer system. This may include name, date of birth, and contact details.
-
Billing Team Solution
Medical billing companies cross-check patient demographics before submitting claims to the insurance companies. They instantly identify and catch errors across all the systems and insurance databases. Coordinating with the front desk teams can help prevent denials and ensure consistency in the future.
-
Complete Insurance Details
-
Effect on Claims
Incorrect insurance information, such as the payer’s name or group number, can lead to claim denials. Such errors may also route your claims to the wrong payer. It results in delays of claim adjudication and also impacts the practice’s cash flow.
-
Billing Team Solution
Medical billing teams verify and validate insurance details before submitting the claims. They verify active coverages accurately and match the payer ID, along with the payer-specific requirements.
-
Policy Validity Check
-
Effect on Claims
If a patient’s policy is inactive or expired at the time of service, the claims are denied instantly. This can result in uncollectible balances for the provider, negatively affecting their revenue cycle.
-
Billing Team Solution
Medical billers confirm policy status and covered services with effective dates before claim submission. They also perform real-time eligibility checks and use automated tools for precision. This helps the billers catch invalid policies in advance and inform the patients about their coverage issues.
-
Avoid Data Errors
-
Effect on Claims
Incorrect formats or general typos can result in payment delays for the providers. It also creates mismatches with the insurance system.
-
Billing Team Solution
Billing teams use medical billing software to help prevent such kind of errors. They may also perform manual audits for high-value claims to ensure compliance and accuracy.
-
Front Desk Accuracy
-
Effect on Claims
The front desk team is considered the first line of defense for medical providers. If they make a mistake in inputting the wrong information, it affects the entire billing process.
-
Billing Team Solution
Billing staff work closely with the front desk personnel to ensure accuracy. They provide regular training to the staff on payer-specific requirements while establishing registration checklists.
-
No Duplicate Records
-
Effect on Claims
Duplicate patient records can lead to confusion and errors in the patient registration process. The insurance companies may deny the claim or raise compliance issues for this type of error.
-
Billing Team Solution
The billing team uses unique identifiers like MRN and DOB to monitor duplicate entries. They instantly coordinate with the Health Information Management teams to maintain a clear record of the patients.
-
Benefits Coordination
-
Effect on Claims
If the Coordination of Benefits (COB) between the primary and secondary insurances is recorded incorrectly, it can lead to denials. This may also lead to overpayments sometimes, which require refunds from the providers.
-
Billing Team Solution
Medical billing companies validate COB during patient registration and update the payer databases with accurate information. This includes ensuring the claims are sent to the primary insurers first. They then handle the secondary submissions according to the treatment requirements.
-
What Role Does Coding Play in the Process?
Medical coding acts as a translator between the clinical services and financial reimbursements. Its primary purpose is to ensure every diagnosis and procedure is accurately assigned to the standardized codes. It helps the payers understand the services properly and reimburse accordingly.
-
Purpose of Medical Coding
Medical coding is essential to create a shared billing language among providers, patients, and insurers. It helps them in consistent data tracking and reporting. Accurate medical coding speeds up the reimbursement process for the provider’s practice.
-
Link Between Services & Billing
Medical coding ensures that the clinical services are transformed into billing charges accurately. It helps the billers properly document the procedures and convert them into claimable services.
-
ICD Diagnosis Codes
International Classification of Diseases (ICD) codes are used to document the patient’s diagnosis. These codes support the medical necessity of the patient’s treatment. It also helps the payers understand the justification of the procedures.
-
CPT Procedure Codes
Current Procedural Terminology (CPT) codes describe the procedures and treatments rendered by the patients. CPT codes reflect the nature of the care, essential for determining the proper reimbursements.
-
HCPCS Supply Codes
The Healthcare Common Procedure Coding System includes the codes for non-physician services like medical supplies, equipment, and ambulance transport. This helps medical billers convert these services into codes understandable by payers.
-
Coding for Reimbursement
Medical coding helps providers get maximum reimbursements if the codes perfectly match payer policies and fee schedules. It ensures the claims meet payer-specific requirements, which may vary across plans.
-
Avoiding Coding Errors
Keeping up with code updates is the key to avoiding claim denials. Outdated coding errors can lead to multiple errors for the providers. Medical billers ensure accurate code selection that aligns with clinical services and documentation.
-
Code Accuracy Compliance
It is essential to adhere to official coding guidelines and ethical standards for compliance and security. Accurate compliance saves the practice from surprise audits and penalties.
-
How Are Claims Submitted to Payers?
Submitting accurate claims to the payers ensures timely reimbursements for the practice. Medical billers help prepare, validate, submit, and track the claims according to payer-specific requirements.
-
Claim Creation Process
Medical billers start the claim creation process by gathering all the relevant data. It includes:
- Clinical documentation
- Charge entry
- Patient information
- Insurance details
- CPT/ICD codes
- Provider information
By ensuring accurate attachments from the start, they can avoid claim denials later.
-
Clearinghouse Integration
Clearinghouses check the claim for any errors before submission. They ensure the claim reaches the correct payer by matching it with payer IDs. If any issue arises, clearinghouses manage the feedback and make edits before final submission.
-
EDI Format Standards
Medical billers utilize billing software that structures a claim with EDI standards. Such standards include the ANSI 837 format. It ensures compatibility with the payer systems. They also comply with HIPAA electronic transaction rules.
-
Portal-Based Submissions
Portal-based submission applies to those payers who do not accept EDI. Medical billers then log into payer-specific portals and submit the claims manually. They can also check eligibility and get follow-up through these portals.
-
Payer-Specific Rules
Medical billers stay updated with unique billing guidelines to customize claim submissions accordingly. These guidelines may include:
- Modifier usage
- Code bundling
- Frequency limits
Accurate alignment with these payer-specific rules is the key to getting reimbursements. Incorrect alignment can lead to rejections or underpayments.
-
Error Scrubbing Tools
Medical billers use error scrubbing tools before claim submission. They scan for:
- Coding mismatches
- Missing fields
- Invalid combinations
The scrubbing ensures accurate claim submission to reduce denials and errors.
-
Submission Confirmation
The billers receive submission confirmation through acknowledgment reports. It confirms the payers have received your claims. The payers also mention if the claim needs to be corrected because of any errors. The billers then resubmit it after necessary corrections.
-
Tracking Claim Status
There are various ways to track claim status. The billers can follow up on the claims through payer portals or manual calls. They monitor for delays, denials, or requests for additional information. Timely action and resubmissions can help prevent cash flow disruption.
-
How Do Providers Handle Denials and AR Follow-Up?
The medical billing team plays an important role in handling denials. They detect, correct, appeal, and recover the practice’s revenue through a structured AR workflow. Here is a brief overview of how they protect the provider’s revenue cycle after claim denials.
-
Identify Denied Claims
Medical billers receive claim denials through either Electronic Remittance Device (ERA) or Explanation of Benefits (EOB) reports. That is why they constantly review these two sources to identify the denied claims.
The provider’s team also categorizes the denial type which includes medical necessity, coding or eligibility. After that, they highlight these claims to correct and resubmit to the insurers.
-
Analyze Denial Reasons
After the billers identify a denied claim, they start to analyze the reason for its denial. They do so by decoding the claim and review the remarks provided by the insurer. The medical billers identify the exact issue and decide whether they need to correct it or file for an appeal.
-
Correct Claim Errors
If the reason for denial was due to an error of coding, coverage, or incorrect information, the billers correct them. They fix the claim and resubmit it quickly to avoid any further delays. Quick corrections bring in fast reimbursements.
-
Initiate Appeal Process
If the denied claim does not have any errors and needs to be reviewed again, the provider’s team files for an appeal. They prepare appeal letters and attach supporting documents with the claim. The team then submits the claim within payer deadline for quicker reimbursements.
-
Track Appeal Status
After submitting the appeal, the billers keep tracking its progress. They escalate stalled appeals to ensure they are not left unresolved. They stay updated with the responses to provide extra documentation if necessary.
-
Monitor Aging Reports
The medical billers use Aging Reports to identify how long each claim is left unpaid. The team then prioritizes follow-ups of the most aged claims to prevent revenue leakage. With timely filing, they are able to protect the practice’s revenue flow.
-
Prioritize High-Value Claims
The providers prioritize high-value claims that bring in more cash. They follow-up those claims to maximize cash flow impact. Recovering the most significant revenue is more important than focusing on low-value denials.
-
Optimize AR Workflow
Billing teams optimize AR workflow to handle claim status. They use task management tools and ensure timely follow-ups to avoid duplication.
-
What Metrics Define a Successful Billing Process?
A successful billing process is defined by the following metrics:
- Quick and accurate claim submissions
- Faster and maximum reimbursements
- Overall healthy revenue flow
-
Clean Claim Rate
A successful claim submission speeds up reimbursement for the practice. It also reflects accurate billing and coding practices. Claims processed in the first attempt reflect the success of a billing process.
-
Claims Paid on First Try
The claims that are paid in full on first submission brings a healthier cash flow for the practice. It means fewer delays and less time spent on denials and follow-up.
-
Days in Accounts Receivable
The lesser the number of days it takes to receive payments, the more financially beneficial it is for the practice.
-
Net Collection Rate
The maximum total revenue collected by the provider reflects a successful billing process. A high net collection rate indicates effective revenue recovery.
-
Charge Lag Time
It is the time between date of service and claim submission. Shorter charge lag indicates faster reimbursements beneficial for the entire revenue cycle of a practice.
FAQs:
- What are the steps of the billing cycle?
The billing cycle typically includes following eight steps:
- Patient Registration
- Insurance Verification
- Medical Coding
- Charge Entry
- Claim Creation & Submission
- Payment Posting
- Denial Management & AR Follow-up
- Reporting & Analysis
- Who handles medical billing in hospitals?
The entire medical billing process is handled by the revenue cycle management (RCM) team in hospitals. This team includes medical billers, coders, and billing specialists.
- What delays claim processing?
A few of the most common reasons for delays in claim processing are:
- Incorrect patient info
- Missing documentation
- Mismatches
- Coding errors
- And more
- What are clearinghouses?
Clearinghouses act as the intermediate system between providers and payers. They receive claims from providers and route them to correct insurers. They also check for any errors or missing info and inform the providers about it.
Partner with Prime Doc Billing Today
Let our experts handle your billing — streamline your revenue cycle and focus on patient care.

Top 10 Benefits of Outsourcing Medical Billing Services
April 15, 2026


 (347) 650-2656
(347) 650-2656


 info@primedocbilling.com
info@primedocbilling.com