Table of Contents
▼Payment Posting in Medical Billing; Definition, Process and Importance
Payment posting refers to the process where the payments received from the insurance companies and patients are recorded accurately with the respective claims. Payment posting involves updating paid amounts, adjustments and outstanding balances to provide a clear view of the revenue cycle of a practice. To ensure accuracy in the payment posting process, several key data points are included in the payment posting which are payer details, patient information and payment details.
The process begins with reviewing remittance details through Explanation of Benefits (EOBs) and Electronic Remittance Advice (ERAs). The EOB and ERA are matched with their respective claims to post payments. The medical billing services company verifies whether the posted amount aligns with the allowed amount to identify discrepancies if any. The remaining balance is either billed to the patient or secondary insurance to ensure timely reimbursements and accurate accounts receivables (AR). The last step includes the reconciliation of transactions to maintain financial consistency and accuracy.
Payment posting plays a critical role in maintaining the financial health of a healthcare practice by ensuring accurate reconciliation of all incoming payments. Payment posting provides clear visibility into cash flow and helps track accounts receivable to identify denial trends and underpayments. Efficient payment posting is essential to prevent revenue leakage and decrease AR days of the revenue cycle.
What is Payment Posting in Medical Billing?
Payment posting in medical billing is the process of recording payments received from the insurance companies and the patients in the billing system. It is a key step in medical billing where EOBs (Explanation of Benefit) and ERAs (Electronic Remittance Advice) are reviewed to extract remittance details such as allowed amount, paid amount, denials, and the patients’ responsibility.
Each payment in the payment posting is matched with the correct claim and date of service to ensure financial accuracy. Payment posting ensures timely reporting, follow-ups and efficient management of accounts receivables in the healthcare organizations.
What are the Key Data Points for Accurate Payment Posting?
They key data points for accurate payment posting includes verifying:
- Payer details which include the insurer’s name, address, and electronic funds transfer (EFT) information.
- Patient Information including their name, date of service (DOS), and claim number.
- Payment details like billed amount, allowed amount, paid amount, patient’s responsibility and contractual adjustments.
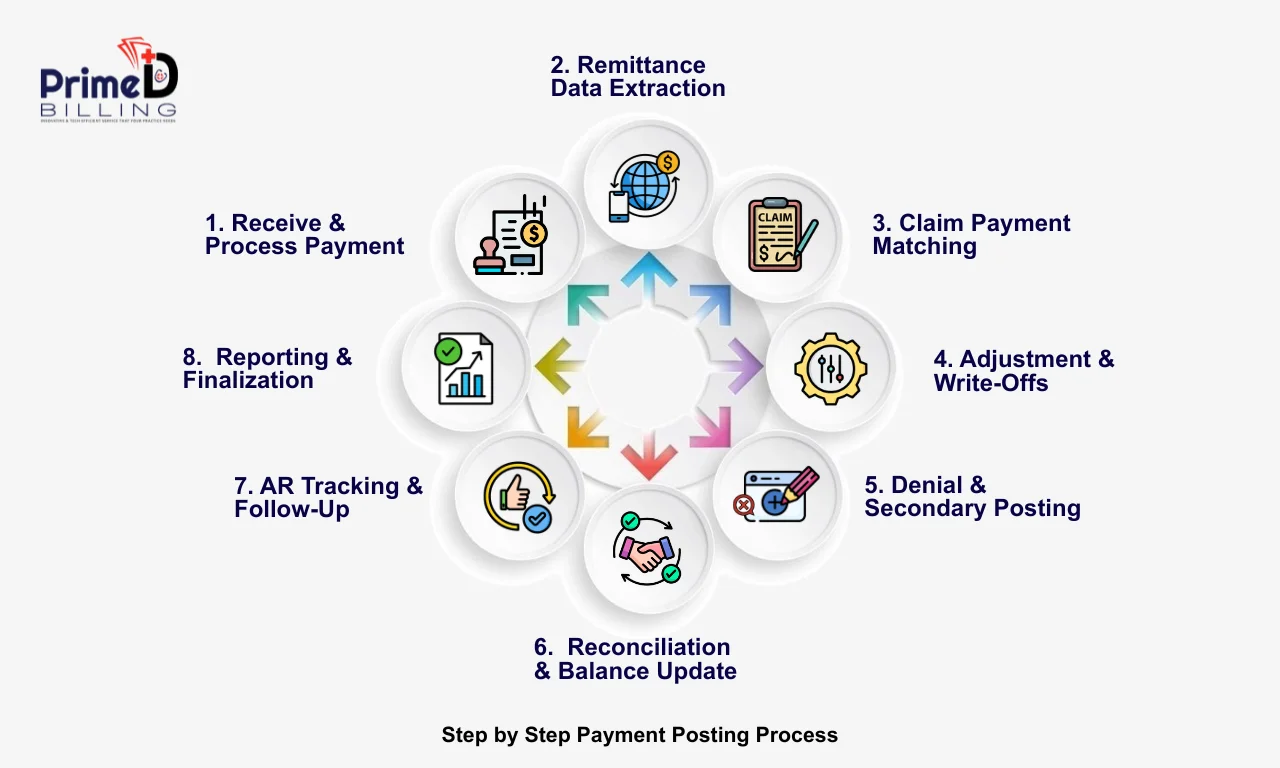
Step by Step Payment Posting Process
Following is the step-by-step process for payment posting in medical billing:
1. Receive and Process Payment Information
The first step for payment posting is to receive payments from the insurance companies and the patients. The payments are received via multiple sources including Electronic Remittance Advice (ERA), Explanation of Benefits (EOB), and Electronic Funds Transfer (EFT). Capturing accurate payments is essential to avoid reconciliation issues.
2. Remittance Data Extraction
Remittance data extraction is the most crucial step of payment posting. The extracted data includes CPT, HCPCS codes, allowed amount, billed amount, paid amount, and patient’s responsibility.
3. Claim Payment Matching
The payments received from the insurance companies and patients need to be matched with the correct claim and patient account to avoid incorrect balances and delayed follow-ups.. The key points to check are claim number, patient name, provider details and the date of service.
4. Primary Payment Posting
The next step is where primary payment posting occurs on the ERA (Electronic Remittance Advice). The primary payment posting includes the amount that the insurance companies and the patients have paid.
5. Adjustment and Write-off Application
The adjustments section explains the reason why the full amount wasn’t paid. The reasons typically include non-covered services, insurer reductions, and contractual write-offs. The reasons for the remaining balance are applied using CARC (Claim Adjustment Reason Codes) and RARC (Remittance Advice Remark Codes).
6. Denial and Underpayment Management
This step identifies the reason for denials, partial payment and underpayments. The medical billing team analyzes the denial codes, and submit the appeal to prevent significant revenue loss of the practice.
7. Secondary Insurance Posting
The remaining balance is billed to the secondary payer if the patient has enrolled with the secondary insurance. This step requires exact posting of coordination of benefits (COB) and accurate transfer of primary insurer’s EOB/ERA details to speed up the reimbursement cycle.
8. Claim and Patient Balance Update
The remaining balance is updated after adjustments and payment posting. The patients’ responsibility is thoroughly calculated to identify copays, deductibles, and coinsurances. Accurate patient billing is essential to reduce billing disputes.
9. Payment Reconciliation
Payment reconciliation is considered the financial control step of the payment posting. The medical biller is required to match Electronic Remittance Advice (ETA) with Electronic Funds Transfer (EFT) to identify the total amount posted and the total amount received.
Daily payment reconciliation is critical to prevent revenue leakage of the practice. Payment reconciliation identifies missing payments early to ensure financial accuracy,
10. AR Tracking and Follow-Up
The claims are categorized into pending, denied and paid to ensure efficient AR management and timely follow-up. The medical billing teams work on denials and track aging accounts to improve cash flow of the practice.
11. Reporting and Finalization
The final step includes reconciliation summary and underpayment analysis to identify payer trends and optimize revenue cycle performance of the practice.
Methods of Payment Posting
Following are the different methods of payment posting in medical billing:
1. Manual Payment Posting
Manual payment posting is the traditional method usually used by small healthcare practices. The billing teams manually enter payment details from EOBs and ERAs into the practice’s billing or practice management system.
2. AI Automated Payment Posting
AI-automated payment posting represents a more advanced method where automation tools and artificial intelligence are used to process Electronic Remittance Advice (ERAs). The automation tools automatically post payments into the system, reducing turnaround times (TAT) and improving accuracy.
3. Manual vs Electronic Payment Posting
The use of manual or electronic payment posting depends on the payer rules and claim volumes. Most healthcare organizations use electronic payment posting for standard payments and manual for complex cases to achieve the perfect balance between efficiency and accuracy.
Insurance vs Patient Payment Posting
| Insurance Payment Posting | Patient Payment Posting | |
| Definition | Insurance payment posting refers to the record of payments received from the insurance companies after claim adjudication. | Patient payment posting refers to the record of payments made by patients, which typically includes self-pay balances, deductibles, or copays. |
| Data Requirements | Insurance payment posting requires the use of CPT codes, payer details and claim numbers. | Patient payment posting requires the date of service, patient ID, and the payment amount. |
| Documentation | The documentations used in the insurance payment posting are EOB (Explanation of Benefits) and ERA (Electronic Remittance Advice) | The documentations required in the patient payment posting are POS transactions, cash or check records, online payments, and receipts. |
| Complexity Level | The insurance payment posting is relatively complex as it involves claim adjudication and payer rules. | The patient payment postings are relatively simpler as it includes a payment entry only. |
Role of Payment Posting in Revenue Cycle Management
Payment posting plays a core function in the revenue cycle management as it ensures that all the payments received are accurately recorded, reconciled and reflected in the system. Payment posting acts as a bridge between claim adjudication and the final revenue of the practice.
One of the most prominent roles of payment posting in RCM is to ensure revenue accuracy, transparency, and cash flow management. Payment posting helps identify underpayments, denials, and discrepancies early so the billing team takes timely action and makes informed decisions.
What are the Payment Posting Challenges faced by Providers?
Some of the most common payment posting challenges faced by the healthcare providers are:
1. Bundled and Split Payment Challenges
Bundling occurs when the insurance companies combine multiple healthcare services into a single payment. Whereas, split payment occurs when the insurers divide single payment of the claim between multiple procedures. Bundled and split payment challenges result in the incorrect balance and underpayments if not allocated properly.
2. Delays in Secondary Insurance Processing
The delays in secondary insurance processing occur when the COB (Coordination of Benefits) is not accurately established. Any delay in forwarding the remaining balance to the secondary payer slows down the entire reimbursement cycle and increases AR days.
3. Prolonged Payment Processing Timelines
Delayed payment processing often occurs because of the inefficient system, staffing limitations, and manual workflows. Delayed identification of underpayments and payment posting impacts the cash flow of the practice.
4. Incomplete or Unclear EOB Information
Incomplete or unclear EOB information creates confusion during payment posting. Missing details like adjustment codes or mismatched claim references increases the likelihood of errors and delays in reconciliation.
5. Underpayments and Reduced Reimbursement Rates
Underpayments is one of the most critical financial challenges of payment posting. The insurance payers often reimburse reduced amounts because of the changes in policy or misapplied coding. The reduced reimbursement rates lead to revenue leakage of the practice.
What are the Best Practices for Accurate Payment Posting?
Some of the most efficient practices for accurate payment posting are:
1. Comprehensive Payment Validation
Proper payment validation helps the providers identify discrepancies early to prevent incorrect balances along with bundled and split payment challenges. The comprehensive payment validation includes details like allowed amount, billed amount, paid amount and the patients’ responsibility.
2. Timely and Efficient Payment Posting
Timely payment posting of both primary and secondary insurances is essential to maintain a healthy cash flow of the practice. Payments need to be posted as soon as they are received to ensure the account balances remain up-to-date. A streamlined workflow helps the healthcare providers stay responsive.
3. Utilization of Automation and Posting Tools
The utilization of automation and posting tools help the providers handle high volumes of transactions timely with accuracy. Automation tools help improve consistency and frees up staff to focus on more complex cases.
4. Routine Auditing and Accuracy Checks
Regular auditing and accuracy checks serves as a quality control mechanism for the practice. Regular audits help identify inconsistencies, errors and missed adjustments to help reduce financial discrepancies over time.
5. Consistent Monitoring of Underpayments
Consistent monitoring of underpayments by comparing payer reimbursements with the contracted rates help identify reimbursement variances early. This step is crucial to maximize revenue of the practice.
What are the Tools and Softwares used for Payment Posting?
Some of the most prime tools and softwares used for payment posting are:
1. Clearinghouses
Clearinghouses are used to match payments to claims, send claim status updates, and process EOB data electronically. Clearinghouses are essential for receiving and processing the electronic remittance data.
A few of the most common clearinghouses are:
- Waystar
- Office Ally
- Change Healthcare
- Availity
2. Practice Management Systems
Practice management systems are used to post payments, update claim and patient balances, track AR, apply adjustments, writeoffs, and generate financial reports. The most common tools of practice management systems include:
- AdvancedMD
- Kareo
- Athenahealth
- Epic Resolute
3. EHR Platforms
EHR platforms connect clinical documentation with the medical billing claims. EHR platforms ensure accurate charge capture and reconciliation to align payments with the patient encounters.
Some of the most common EHR platforms are:
- NextGen EHR
- Epic EHR
- Athenahealth EHR
4. Automation Tools
The advanced revenue cycle management companies use automation tools for faster payment posting. The automation tools help the practice capture underpayment detection, AI claim matching, automated reconciliation, and reduced manual entry errors. The most widely known automation tools in payment posting are:
- InstaMEd
- R1 RCM tools
- nThrive automation tools
How does Prime Doc Billing help you in Accurate Payment Posting?
Prime Doc Billing helps you ensure accurate payment posting by aligning with your structures revenue cycle workflows. Our team carefully processes EOBs and ERAs to extract remittance details such as adjustment codes, payment amounts, and denial reasons.
Our team matches each payment to the correct claim using identifiers like claim number, provider details, and the date of service. We proactively identify underpayments and denials to prevent revenue leakage and enhance payment posting accuracy of the practice.
Frequently Asked Questions
1. What is the role of a payment posting specialist in payment posting?
A payment posting specialist accurately records payments from insurance companies and the patients into the billing systems.
2. What is the impact of payment posting on AR days?
Timely and accurate payment posting decreases Accounts Receivable (AR) days, removes backlogs and increases cash flow of the practice.
3. What common mistakes people make in payment posting?
Some of the most common mistakes the people make in payment posting are failure to identify underpayments, duplicate postings, missing or incorrect adjustments and incorrect payment allocation.
4. How are charges captured for a patient visit?
The provider documents all services during or immediately after the visit. The billing team reviews that documentation, identifies all billable elements, and enters them into the billing system. A coder assigns CPT and ICD-10 codes and the claim is submitted. With real-time charge capture tools, providers enter charges directly at point of care, reducing lag between service delivery and billing.
5. What are the benefits of payment posting?
Efficient payment posting helps improve cash flow, reduces claim denials, identify underpayments, and enhances financial reporting of the practice.
5. What are payment posting services?
Payment posting services are the outsourced solutions where the medical billing team handles the posting of payments and reconciliation. The payment posting services help improve accuracy and speed up the revenue cycle of the practice.
Partner with Prime Doc Billing Today
Let our experts handle your billing — streamline your revenue cycle and focus on patient care.